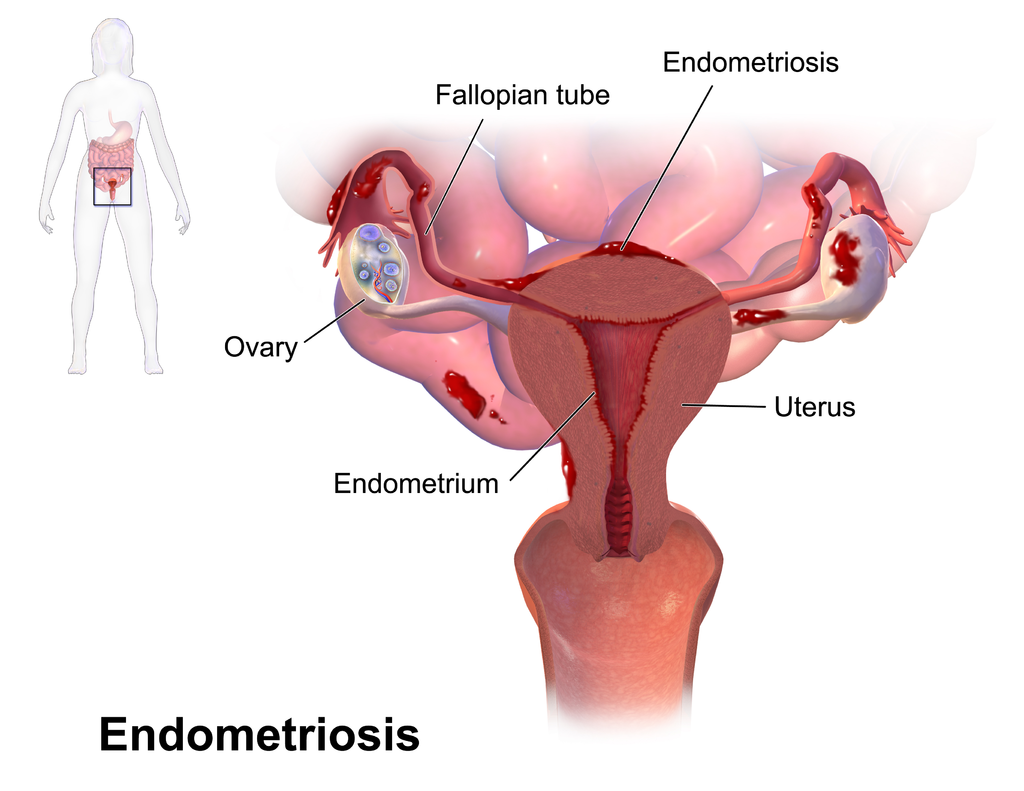
*In todays blog about endometriosis excision surgery, I am writing from personal experience and do not claim to have medical expertise or to be able to give medical advice.
Many of you know that I was diagnosed with severe stage 4 endometriosis around 2 years ago, after at least 10 years of pain and suffering from the disease. I’d like to share my story, and explain why I recommend excision surgery with a specialist as the best way forward for anyone with severe and extensive endometriosis.
Diagnosing Endometriosis
I had been seeing my GP on and off since I was 16 years old – I was 36 when finally officially diagnosed with endometriosis! Needless to say its a disease difficult to diagnose, mainly because many of the symptoms overlaps with so many other conditions – fibroids, IBS, cancer, Chrones disease. Endometriosis is essentially womb lining growing outside of the womb in places where it should not be, often leading to cysts, lesions and adhesions.
The only real way to diagnose endometriosis is by having a diagnostic laparoscopy which I finally had at the age of 36. It showed extensive disease on several organs and showed that my organs had actually fused together with lesions. My ovaries had attached themselves to my bowel wall! (This is one of the reasons why I now ).
I was finally referred to Ediosagie at Manchester St Mary’s following paying for a private diagnosis with him and the Alexander BMI. Immediately on examining me, he identified extensive disease and at least two operations.
Hormonal Control of Endometriosis
In the run up to the operation, I was offered Lupron, a strong hormonal injection that is used in late stage prostate cancer that would have thrusted me into an early menopause – no thank you! I decided on excision surgery and went on the NHS waiting list, which took 18 months to get. In between, I was on extensive medication including cocodomol and laxatives.
Excision Surgery for Endometriosis
I finally had excision surgery with Ediosagie on 1st February. I was in theatre for almost 6 hours and had endometriosis removed from my bowel, bladder, ovaries, ureters and abdominal wall. Just two weeks later I was eating full meals despite not being able to eat properly for 2 years. I was out and about, back working and feeling better than I had in years, just 3 weeks post op.
Yes, there are risks to every surgery, and mine was not without complications (urinary retention for a week post op). However, the point was that I could not have continued my life as I was. The pain was so severe that I couldn’t work or travel. I consented to a laparotomy (when the open you up with a large scar) and a temporary ileostomy (bag to collect your waste!) Thankfully, they didn’t have to do these procedures, but if they had, I would still have been glad to have the surgery. My quality of life has drastically improved since excision surgery.
Medication for Endometriosis
The default for a woman with endometriosis is drugs, rather than surgery. There may be many reasons for this.
Perhaps her pain can be controlled by paracetamol or ibuprofen. However, endometriosis pain is usually much more serious and needs cocodomol, tramadol and morphine to barely touch it. The drugs are not curing or solving the problem, they are simply masking it. What’s more, opiate based pain relief tends to exacerbate endometriosis symptoms including constipation, so can be counter-productive.
Other than paid killers, the next go to medication for endo is often hormonal, because endometriosis is hormonally fuelled. So oral contraceptives or deep provera are often recommended. A stronger option would be lupron or prostap, shutting down your ovaries. All well and good….
But what about for a woman who wants to get pregnant? Well, it’s not really an option for women who want a family as these drugs will stop that from happening. Many women’s personal wishes are ignored or not taken into account. In addition, depression and anxiety are side effects of many hormonal drugs, so their physical health may improve only to see a deterioration in their mental health.
My opinion is that if endometriosis is stage 3/4 and or preventing them from working, travelling or having a sexual relationship, they should be offered a laparoscopy and ultimately, laparoscopic excision.
Why Endometriosis Excision Surgery should be Gold Standard for Extensive Disease
Some surgeons will recommend a hysterectomy, which, in some cases, may be appropriate, particularly if a woman has completed her family. However, if the endometriosis is found in other areas such as on the bladder or bowel and the womb is removed, symptoms will continue. It’s almost like diagnosing liver cancer and removing the pancreas! So get specialist advise and a laparoscopy before making any big decisions.
Lena Dunham (actress) has recently had a hysterectomy for endometriosis at the age of 31, and she is now speaking out about the disease and raising awareness. It’s true that more people need to know about it and understand it, including GPs.
My preferred alternative to a hysterectomy or drugs was endometriosis excision surgery. Endometriosis excision surgery is often lengthy as the endometriosis has to be meticulously removed bit by bit, often from several areas of the pelvis and from several organs in stage 4 endo. It’s better than ablation (burning or lazering) as the endo is less likely to come back. Although endometriosis can recur after excision surgery, it is less likely, or it may return over a longer period of time.
Endometriosis excision surgery has a relatively high success rate and low complication rate. The thing is, only specialists can perform this – you won’t get good excision from a regular ob gyn. So, if you want excision, look for a specialist BSGE centre with an endometriosis surgeon.
Thankfully, I’m writing this blog pain free and ready to travel to Malta and Thailand. I finally feel like I have a future ahead of me thanks to my fabulous surgeon Ediosagie.
You might also like to read my article about travelling with endometriosis or International Womens Day 2018.